Tooth Infection?
Here's What to Do — Fast.
Gentle, same-day emergency dental care for patients in Oxnard, Camarillo, Ventura, Thousand Oaks & Port Hueneme.
Serving Oxnard • Camarillo • Ventura • Thousand Oaks • Port Hueneme
If you have facial swelling, difficulty breathing or swallowing, or a high fever alongside tooth pain — go to the emergency room immediately. These can be signs of a spreading infection. For all other tooth infections, call us first at (805) 486-6327.
A toothache that throbs. A jaw that looks puffy. A weird taste you can't get rid of. If any of that sounds familiar, you may be dealing with a tooth infection — and we know how scary and painful that can feel.
The good news? If you act fast, you have real options. Many patients who call us early are able to save their tooth, avoid serious complications, and walk out the same day feeling dramatically better. This guide walks you through everything: how to recognize a tooth infection, what your treatment choices actually look like, and what happens if you wait.
We serve patients across Ventura County — from Oxnard and Port Hueneme to Camarillo, Ventura, and Thousand Oaks. If you're dealing with this right now, don't wait until the end of the article to call us.

Tooth infections are one of the most painful dental emergencies — but acting fast gives you real options.
What Is a Tooth Infection, and Why Is It Urgent?
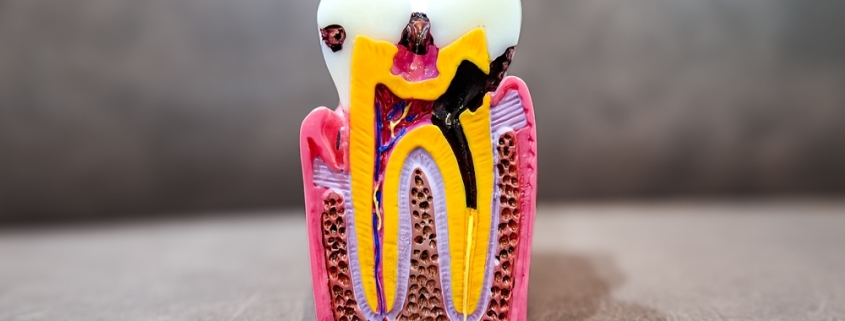
A tooth infection — also called a dental abscess — happens when bacteria invade the inside of a tooth or the surrounding gum tissue. This most often occurs because of untreated tooth decay, a cracked tooth, or gum disease that has progressed far enough to allow bacteria to reach the tooth's root or pulp (the soft tissue inside).
Unlike a skin infection that your immune system might manage on its own, a dental abscess almost never resolves without treatment. The infection is enclosed inside hard tooth structure, which means your body has very little ability to fight it off. Left alone, it spreads — to the jawbone, the neck, and in serious cases, into the bloodstream in a life-threatening condition called sepsis.
This is why dentists take tooth infections seriously, and why we always say: call us today, not next week.
How do I know if I have a tooth infection?
The symptoms can range from obvious to subtle. Here are the most common signs our Oxnard and Ventura County patients describe when they call us:
- A persistent, throbbing toothache — often worse when you lie down
- Sensitivity to hot or cold that lingers well after the temperature is gone
- Swelling in your face, cheek, or jaw
- A bad or bitter taste in your mouth, sometimes accompanied by pus
- A pimple-like bump on your gums near the painful tooth (called a fistula)
- Fever, fatigue, or swollen lymph nodes in your neck or jaw
- Pain that radiates to your ear, jaw, or neck
Sometimes, a tooth that was once painful suddenly stops hurting. This does not mean the infection healed — it often means the nerve has died. The infection is still there and still spreading.
Can a tooth infection go away on its own if I just wait it out?
No — and this is one of the most important things to understand. A dental abscess will not resolve without treatment. It may seem to quiet down for a few days, especially if you take over-the-counter pain relievers or if the abscess drains on its own. But the source of infection remains, and it will flare again — often worse than before.
Every day you wait is a day the infection has to spread. Patients who come to us in Oxnard after waiting weeks often have more complex situations than those who called us at the first sign of pain. Early treatment means more options, simpler procedures, and a faster recovery.
Your Treatment Options — What Acting Fast Gets You
This is the part most people want to know: what is actually going to happen when you come in? The answer depends heavily on how far the infection has progressed. Here is an honest breakdown of what your options look like at different stages.
Antibiotics + Monitoring
If the infection is caught in its earliest stages — before it has fully penetrated the tooth pulp — antibiotics can be prescribed to control the bacterial spread. This is a temporary measure, not a cure. You will still need to address the underlying cause (usually a cavity or crack), but antibiotics buy time and reduce the immediate risk.
This option is most available to patients who call us at the first sign of symptoms. Patients in Camarillo, Ventura, Thousand Oaks, and Oxnard who come in early often avoid the more involved procedures below.
Root Canal Therapy
When the infection has reached the pulp (the inside of the tooth), a root canal is typically the best path to saving your natural tooth. During the procedure, we remove the infected pulp, thoroughly clean and disinfect the inside of the tooth, and seal it. A dental crown is usually placed afterward to protect it.
Root canals have an unfair reputation. With modern anesthesia and a gentle approach, the procedure is far more comfortable than most patients expect. Many of our Oxnard and Ventura County patients tell us it was nothing like they feared — and that the relief afterward was immediate.
Root canal therapy is covered in detail in our root canal and crown guide if you want to learn more.
Tooth Extraction
In some cases, when an infection has severely damaged the tooth structure or spread too extensively, extraction becomes the safest option. We always try to save a natural tooth first, but when saving it is no longer realistic, removing it quickly stops the infection and relieves pain.
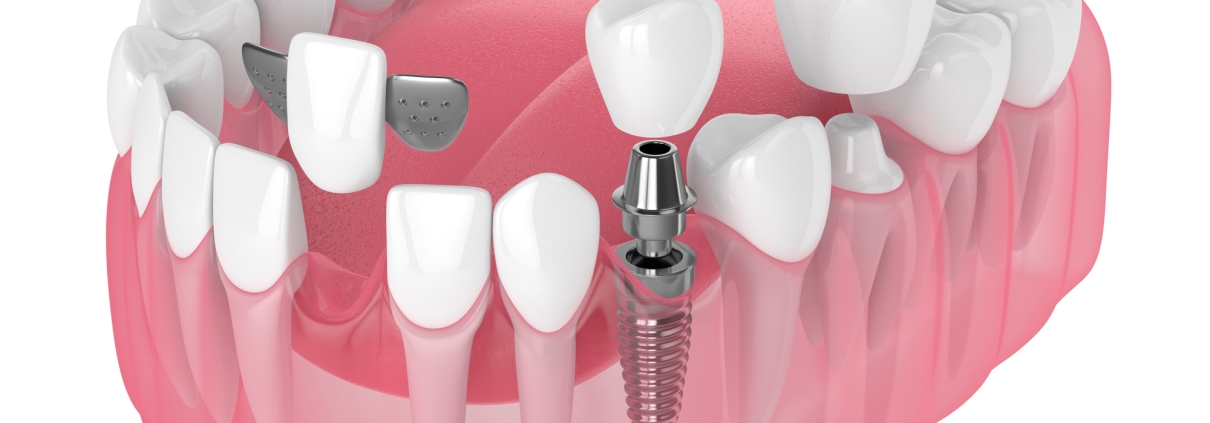
If a tooth does need to be extracted, we will talk through your replacement options — including dental implants, bridges, or partial dentures — so you know exactly what the path forward looks like.
Do I definitely need a root canal if I have a tooth infection?
Not always. It depends on how deep the infection has gone. If it has reached the pulp of the tooth, a root canal is typically the right treatment. If you caught it earlier, antibiotics and a filling or crown may be enough.
The only way to know for sure is an exam and X-rays. We will not recommend a root canal unless it is genuinely the right treatment for what we find. And we will always explain what we see, show you your X-rays, and give you the information you need to make a confident decision.
Will it hurt? I'm terrified of dental procedures.
We hear this every day, and we take it seriously. Our entire practice was built around patients who are nervous, who have had bad experiences elsewhere, or who have been avoiding the dentist for years because of fear.
Here is what we do differently: we apply topical numbing gel before the anesthetic needle, so even the first step is as gentle as possible. We explain each step before we do it. We check in with you throughout. You are always in control — if you need a break, you get one, no questions asked.
The pain of an untreated tooth infection is real. The procedure to treat it is not nearly as bad as most people expect. And the relief after? That part our patients do not forget.
What Happens If You Wait
We are not here to scare anyone — but we also want to be honest with you, because we care about the people who come to us. Untreated tooth infections do not stay in your tooth. Here is what can happen when bacteria spread:
Jaw Bone Damage
Infection spreading into the jawbone (osteomyelitis) can cause bone loss that requires surgery to treat.
Spreading Abscess
Abscess can spread to soft tissue in the neck and floor of the mouth — a serious condition called Ludwig's angina.
Sepsis
In rare but real cases, dental infections can enter the bloodstream and cause sepsis — a medical emergency requiring hospitalization.
Tooth Loss
A tooth that could have been saved with a root canal early on may need to be extracted if infection destroys enough tooth structure.
I can't afford a root canal right now. What should I do?
Please call us anyway. Cost should never stop someone from getting care they need, and we have options to help. Most major PPO insurance plans cover a significant portion of root canal treatment and emergency dental visits. Our front office team will review your benefits before treatment so you know exactly what to expect.
For out-of-pocket costs, we offer flexible financing through Cherry Payment Plans, which allow you to break treatment costs into manageable monthly payments. We also have a Membership Plan for patients without insurance. We would rather find a way to make treatment work for you now than have you wait until the situation is far more complex — and far more expensive.
What to Do Right Now — Step by Step
If you think you have a tooth infection, here is a practical list of what to do today:
-
1
Call us. Reach Oxnard Gentle Dentistry at (805) 486-6327. We offer same-day and next-day appointments for urgent dental issues. If you prefer, you can also book online or text us. Getting on our schedule today is the single most important step.
-
2
Manage pain at home in the meantime. Over-the-counter pain relievers like ibuprofen (Advil) or acetaminophen (Tylenol) can help reduce pain and inflammation. Ibuprofen tends to work better for dental pain because it also reduces swelling. Do not place aspirin directly on the gum — it can cause a chemical burn.
-
3
Rinse gently with warm salt water. Half a teaspoon of salt in 8 oz of warm water can help draw out some of the infection and soothe surrounding tissue. Do this a few times a day, but do not use it as a substitute for calling us.
-
4
Avoid the following. Don't apply heat to the outside of your face — it can encourage the infection to spread. Avoid very hot or very cold foods and beverages. Don't poke or press the swollen area.
-
5
Go to the ER if symptoms escalate. If you develop difficulty breathing or swallowing, significant facial swelling spreading toward your eye or neck, high fever, or feel generally unwell — go to the emergency room immediately. These are signs the infection is spreading beyond the tooth.
I live in Camarillo / Ventura / Thousand Oaks / Port Hueneme. Can I still come to Oxnard Gentle Dentistry?
Absolutely. We see patients from across Ventura County every day. Our office at 300 E Esplanade Drive in Oxnard is centrally located and easy to reach from Camarillo, Ventura, Thousand Oaks, and Port Hueneme. Most patients from surrounding cities are with us within 20 to 30 minutes.
We know that when you have a tooth infection, driving a little further for a practice you can trust is worth it. Many of our most loyal patients made that drive once during an emergency — and never went back to their old dentist.
I haven't been to the dentist in a long time and I'm embarrassed. Will you judge me?
Not for a single second. We hear this from so many patients — people who avoided the dentist for years because of fear, cost, a bad experience, or life just getting in the way. We are genuinely not here to lecture you or make you feel guilty.
What brought you in today is what matters. We will do a gentle exam, show you what we find in plain language, and give you choices. You are always in control of your treatment. No pressure, no shame — just care.
Serving Patients Across Ventura County
Oxnard Gentle Dentistry is located at 300 E Esplanade Drive, Suite 1600, Oxnard, CA 93036, and we regularly see patients from:
Oxnard
Our home base. Walk-ins and same-day emergency appointments welcome for Oxnard residents dealing with tooth pain or infection.
Camarillo
Just a short drive down the 101. Many Camarillo patients choose us for emergency dental care and ongoing family dentistry.
Ventura
We see patients from Ventura regularly — for emergency treatment, root canals, crowns, and more.
Thousand Oaks
Thousand Oaks patients searching for a gentle, anxiety-friendly dental office make the drive to us — and keep coming back.
Port Hueneme
Minutes away from our office. Port Hueneme residents with dental emergencies are always welcome.
All of Ventura County
Wherever you are in Ventura County — if you're searching for an emergency dentist near you, we're here.
Don't Wait on a Tooth Infection
The sooner you call us, the more options you have. Same-day and next-day appointments are available for patients dealing with tooth pain, swelling, or suspected infections. We serve Oxnard, Camarillo, Ventura, Thousand Oaks, Port Hueneme, and all of Ventura County.
Mon – Thu | 8:00 AM – 5:00 PM | Most PPO Insurance Accepted